
COVID-19 Vaccines: A Message of Hope
By Aurora Pop-Vicas
“For I know the plans I have for you,” declares the Lord, “plans to prosper you and not harm you, plans to give you hope and a future.” Jeremiah 29:11
The year 2020 has engaged the world in a war against an invisible enemy – a virus that has infected more than 90 million and killed almost 2 million people so far.1 By now we all know someone who has either died or been hospitalized with severe COVID-19 illness. Most of us have seen our lives upended by job losses, financial insecurity, travel restrictions, and social distance measures that clouded our holidays, took a toll on our relationships, and left our mental health precariously fragile. Fortunately, there is palpable hope on the horizon. The first COVID-19 vaccines have become available shortly before Christmas, and millions of frontline workers and nursing home residents have already received their first dose in several countries before the end of the year. Soon, the vaccine will likely be offered to the public, including the readers of this journal, should they choose to accept it.
The fact that we now have a powerful weapon that can tip the outcome of this war heavily in our favor should be a source of unadulterated joy for all, one would think. Unfortunately, my Facebook page continues to be inundated by comments and posts oozing disinformation, fear, doubt, and negativity – too often from individuals loudly proclaiming their “Christian faith” in the same breath, I am sorry to say. Clearly not everyone views scientific wonders of incredible benefit to humankind as cause for celebration. And although in other controversial circumstances we can afford to reserve judgement and let things play out for a while before we take a stance, we do not have the luxury to wait and see now. The stakes are too high, as our choices vis-à-vis COVID-19 vaccines will largely impact the outcome of 2021 for all of us.
Vaccine Precursors
Vaccine development is undoubtedly one of the most fascinating historical achievements. It first started as a means of preventing smallpox, a disease which, although unknown today, has plagued the world for millennia, bringing down empires and wiping-out civilizations. The smallpox epidemic of 108 AD, for example, triggered the decline of the Roman Empire by killing almost 7 million of its citizens.2 The introduction of smallpox into the New World with the arrival of the Spanish and Portuguese conquistadors hastened the demise of the Aztec and Incan Empires. The intentional use of smallpox as a biological warfare agent by the British during the French Indian War (1754 – 1767) decimated a large segment of the American Indian tribes on the eastern coast of North America.3 Meanwhile, in early18th century Europe, the “speckled monster” killed 400,000 people each year, leaving survivors blind or disfigured for life.4
The precursor to the first vaccine was an inoculation practice called “variolation,” (from variola, the name of the smallpox virus), which gained popularity in the 18th century. In variolation, fresh material obtained from a ripe pustule of someone suffering from smallpox was subcutaneously inoculated, usually via a lancet, onto the arm or leg of a person who never had smallpox. This caused a lighter form of disease that self-resolved and subsequently rendered the variolation recipient immune.5 Variolation was widely practiced in the Ottoman Empire and witnessed by Lady Mary Wortley Montague during her stay in Istanbul as the wife of the English ambassador to the Sublime Porte. Lady Montague, who had lost her beauty to smallpox, submitted her 5-year-old son to variolation at the sultan’s court in 1718. She then had her 4-year-old daughter inoculated in front of the royal court physicians upon her return to England in 1721.
After successful trials on a widely diverse population of prisoners, orphans, and the two daughters of the Princess of Wales, the practice became widely used among nobility and commoners alike throughout Europe and the New World colonies.6 There were drawbacks, of course: about 2-3% of variolated persons died of smallpox or became infected with syphilis and tuberculosis – not surprising given the crude manner of the inoculation. Nevertheless, the mortality rate of variolation-associated smallpox was merely 1/10th the mortality rate associated with naturally occurring smallpox.6
Vaccines Arrive: Smallpox Eradicated
The first vaccine was developed by Edward Jenner, an English physician, in 1796. As a 13-year-old teenager and apprentice to a country surgeon, he had overheard a dairymaid declare “I shall never have smallpox, for I have had cowpox. I shall never have an ugly pockmarked face.”7 Many years later, after Jenner started his own medical practice, he postulated that the deliberate transmission of cowpox from one person to another could protect against smallpox. To test this theory, he inoculated material from a dairymaid’s cowpox sore into the arm of an 8-year-old boy, the son of his gardener. One can only imagine the conversations between the doctor, the gardener, and the boy. The boy developed mild symptoms (a low-grade fever, axillary discomfort, loss of appetite), and made a full recovery within 10 days. A few months later, Jenner inoculated the boy with smallpox material repeatedly, but the boy never developed disease.5
Although his initial writings were met with skepticism, by the time Jenner published his 1801 treatise “On the Origin of the Vaccine Inoculation,” detailing his experiments with “vaccination” (from Latin vacca = cow, and vaccinia = cowpox), he had gained important allies within the medical community, and subsequently convinced the British Parliament to fund his scientific work.5 In 1800, Edward Jenner’s vaccine material made its way to Benjamin Waterhouse, a physician and professor at Harvard Medical School, who vaccinated four of his children, implemented vaccination throughout New England, and appealed to then vice-president Thomas Jefferson with a “prospect of exterminating smallpox.” Thomas Jefferson expressed his support for the project in a letter dated Christmas Day, 1800. He continued to champion public vaccination throughout the United States after he became president the next year. In 1813, US Congress established the National Vaccine Institute, with Benjamin Waterhouse appointed to a leadership role.8
These initial efforts paved the way to the eventual eradication of smallpox. After the disease was eliminated from North America in 1952 and from Europe in 1953, the World Health Organization (WHO) began a global eradication plan in 1959. At first, lack of funds, commitment, and resources from the most affected countries, combined with significant vaccine supply shortages allowed smallpox to continue unabated. Ultimately, improvement in vaccine technology and production, creation of effective infection surveillance systems, and intensified mass vaccination campaigns proved successful. On May 8, 1980, almost two hundred years after Jenner’s dream that “the annihilation of the smallpox, the most dreadful scourge of the human species, must be the final result” of his vaccine discovery, the WHO declared smallpox eradicated, and the world celebrated what, until now, has been considered the highest international achievement in public health.9
Vaccines for COVID-19
We now find ourselves at another historical tipping point – in the middle of an enormous global health crisis, but within reach of the most promising public health tool to overcome it. The discovery, trial, approval, and international distribution of COVID-19 vaccines that are 95% effective in less than one-year (a process which usually takes 4-10 years), is an extraordinary triumph of global cooperation and scientific progress. Of course, this success is the end-result of enormous sacrifice and passion poured over decades-long research by amazing scientists, with visionary investment from multiple governments, companies, and private foundations who provided billions in financial support for these efforts.
Vaccines generally work by introducing into the human body a viral protein or an inactivated viral fragment (called an antigen), which the body recognizes as foreign, triggering an immune response meant to destroy the invading substance. Memory cells formed in the process are maintained dormant after this initial encounter. If the vaccinated person is subsequently exposed to the natural virus during an epidemic, for example, memory cells quickly activate the body’s immune response against an invader they are already familiar with, preventing the immunized person from being infected or becoming ill.10
Two of the COVID-19 vaccines currently in use rely on a novel approach which introduces the genetic material that instructs the cell to produce the intended viral antigen, rather than directly administering the intended antigen, as done with conventional vaccines. This novel messenger RNA (mRNA) technology has been the focus of intense research over the last 10-15 years, often in the context of cancer vaccines. It allows for the chemical synthesis of vaccine candidates within a few days, as opposed to the longer time required by traditional vaccine biotechnology. Prior work on related coronaviruses such as those causing severe acute respiratory syndrome (SARS) and Middle East respiratory syndrome (MERS) has established that the best vaccine antigen is the viral spike protein. Once the genome of the SARS-CoV-2 virus causing COVID-19 was sequenced and made internationally available in January of 2020, and just a few days after the first pneumonia cases reported in Wuhan, China, scientists could create a vaccine antigen by tuning the appropriate mRA genetic sequence that codes for this viral spike protein.11
Scientific Heroes
The stories of the scientists at the forefront of this technology with potential to revolutionize the vaccinology field are quite remarkable. For example, Katalin Kariko, a Hungarian biochemist, has worked on developing RNA therapies for 40 years. She started in her 20s while earning her PhD at the University of Szeged, but soon reached a dead-end due to lack of research funding. She fled communism, immigrating to the US in the 1980s with her husband and 2-year-old daughter, hiding the $1,200 received from selling the family car in her daughter’s teddy bear. She continued her RNA work at Temple University and, later, at University of Pennsylvania. The scientific community of the 1990s often dismissed her RNA research, which made securing laboratory grant funding challenging. She persevered despite being demoted from her tenured faculty track position.
The situation changed in 1997 in front of a department’s photocopier where she serendipitously met Drew Weissman, a newly arrived MD-PhD immunologist working on HIV vaccines. The two scientists realized they have common research interests and started collaborating, successfully publishing in 2005 groundbreaking work on how synthetically modified bacterial or viral RNA can stimulate human immune responses.12 They later showed that enveloping synthetic RNA in a coat of lipid nanoparticles prevents premature degradation and facilitates entry into human cells, making it a feasible therapeutic. This strategy was used in 2020 to develop the mRNA COVID-19 vaccines by two biotech companies that proved instrumental in the vaccine race – Moderna in US, and BioNTech in Germany. Katalin Kariko, now a senior VP at BioNTech, is seeing her life-long dream come true at the age of 65. She is likely to share a Nobel Prize with Dr. Weissman in the future. Her daughter has already known success of her own, winning two Olympic gold medals as part of the US rowing team in 2008 and 2012.13
The story of Dr. Ugur Sahin and his wife, Dr. Ozlem Tureci, the physician couple owning BioNTech, is no less impressive. Although they are now billionaires, they live an understated life, focus on work aimed at finding new treatments and saving lives. They reside in a modest apartment, bike to work, and do not own a care They both come from Turkish families immigrated to Germany. Dr. Sahin, whose parents worked for a Ford company in Cologne, became a physician and earned a doctorate in 1993 from the University of Cologne for work on immunotherapy in tumor cells. Dr. Tureci, the daughter of a physician originally from Istanbul, initially wanted to be a nun, but ultimately followed in her father’s footsteps. She met Dr. Sahin while they were both working on a hospital oncology ward in Homburg. On the day of their wedding, the couple returned to their research lab shortly after the ceremony.
They founded BioNTech in 2008, and focused primarily on finding immunotherapies for cancer, including through vaccines based on mRNA technology.14 In January of 2020, when Dr. Sahin read a paper in The Lancet describing the spread of the novel coronavirus causing pneumonia throughout China,15 he became convinced that a pandemic is unfolding, and summoned his scientists from vacation to begin working on a vaccine. They soon identified several promising candidates but needed help to manufacture the vaccine at mass-scale and conduct large international clinical trials. The company had been collaborating with Pfizer since 2018 on flu vaccine research. As a result, Dr. Sahin had developed a unique friendship with Albert Bourla, the Greek CEO of Pfizer. In March 2020, they agreed to work together on COVID-19 vaccine development.14 In December 2020, they published the results of their collaboration in the New England Journal of Medicine: a 95% vaccine efficacy in a double-blinded, randomized, placebo-control trial that enrolled almost 44,000 adults.16,17 At the same time, the second vaccine relying on mRNA technology, developed by Moderna in US, reported a 94% efficacy in a trial of 30,000 participants.18
A Message of Hope
We begin the year 2021 in hope. We have safe and effective vaccines, produced through incredible efforts of international collaboration, with enormous public and private funding, showing what humans can accomplish when they come together in times of crisis. For those of us with faith in God, we undoubtedly see God’s hand at work, as we contemplate how the pieces perfectly complete the puzzle of history.
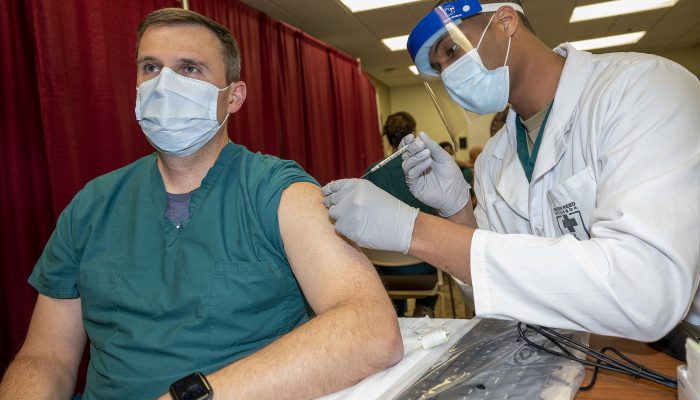
As an infectious disease physician, I was fortunate enough to receive my first COVID-19 vaccine dose in December 2020. Despite having a history of severe allergies, including anaphylaxis, I experienced no vaccine side effects, other than a mildly sore arm for a day. The psalmist’s words written thousands of years ago once again rang true: I will say of the Lord, He is my refuge and my fortress, my God, in whom I trust.…I will not fear the terror of night, … nor the pestilence that stalks in the darkness, nor the plague that destroys at midday. (Psalm 91)
— Aurora Pop-Vicas, MD, MPH is Assistant Professor in the Department of Medicine, Division of Infectious Disease, at the University of Wisconsin School of Medicine and Public Health, Madison, WI
References:
1. John Hopkins Coronavirus Resource Center. Available at: https://coronavirus.jhu.edu/map.html; last accessed January 11, 2021.
2. Littman RJ, Littman ML. Galen and the Antonine plague. Am J Philol 1973;94:243–255.
3. Henderson DA, Inglesby TV, Bartlett JG, Ascher MS, Eitzen E, Jahrling PB, Hauer J, Layton M, McDade J, Osterholm MT, O’Toole T, Parker G, Perl T, Russell PK, Tonat K; Working Group on Civilian Biodefense. Smallpox as a biological weapon: medical and public health management. JAMA 1999;281: 2127–2137.
4. Barquet N, Domingo P. Smallpox: the triumph over the most terrible of the ministers of death. Ann Intern Med 1997;127(8 Pt 1):635–642
5. Willis NJ. Edward Jenner and the eradication of smallpox. Scott Med J 1997;42:118–121.
6. Stefan Riedel. Edward Jenner and the history of smallpox and vaccination. Baylor University Medical Center Proceedings 2005; 18: 21-25
7. Parish HJ. Victory with Vaccines: The Story of Immunization. Edinburgh: E & S Livingstone, 1968.’
8. Underwood EA. Edward Jenner, Benjamin Waterhouse and the introduction of vaccination into the United States. Nature 1949;163:823–828.
9. Centers for Disease Control and Prevention. History of Smallpox. Available at: https://www.cdc.gov/smallpox/history/history.html; last accessed January 8, 2021
10. World Health Organization. How do vaccines work? Available at: https://www.who.int/news-room/feature-stories/detail/how-do-vaccines-work; last accessed January 9, 2021.
11. Philip Ball. The lightning-fast quest for COVID-vaccines – and what it means for other diseases. Nature news feature, December 18, 2020. Available at: https://www.nature.com/articles/d41586-020-03626-1; last accessed January 9, 2021.
12. Katalin Kariko, Michael Buckstein, Houping NI, Drew Weissman. Suppression of RNA Recognition by Toll-like Receptors: The Impact of Nucleoside Modification and the Evolutionary Origin of RNA. Immunity, August 2005; 23 (2): 165 – 175.
13. Stephanie Trouillard. Katalin Kariko, the scientist behind the Pfizer Covid-19 vaccine. Available at https://www.france24.com/en/americas/20201218-katalin-kariko-the-scientist-behind-the-pfizer-covid-19-vaccine; last accessed January 8, 2021.
14. David Gelles. The Husband-and-Wife Team Behind the Leading Vaccine to Solve Covid-19. The New York Times, November 10, 2020. Available at https://www.nytimes.com/2020/11/10/business/biontech-covid-vaccine.html; last accessed January 8, 2021.
15. Chen Wang, Peter W Horby, Frederick G Hayden, George F Gao. A novel coronavirus outbreak of global health concern. The Lancet February 15, 2020; 395 (10223): 470-473. Published online January 24, 2020.
16. Fernando P. Polack, Stephen J. Thomas, Nicholas Kitchin et al. Safety and Efficacy of the BNT162b2 mRNA COVID-19 Vaccine. New England Journal of Medicine, December 31, 2020; 383:2603-2615
17. Jared Hopkins. How Pfizer Delivered a Covid Vaccine in Record Time: Crazy Deadlines, a Pushy CEO. The Wall Street Journal, December 11, 2020. Available at: https://www.wsj.com/articles/how-pfizer-delivered-a-covid-vaccine-in-record-time-crazy-deadlines-a-pushy-ceo-11607740483; last accessed January 8, 2021.
18. Vaccines and Related Biological Products Advisory Committee Meeting December 17, 2020 FDA Briefing Document Moderna COVID-19 Vaccine. Available at: https://www.fda.gov/media/144434/download; last accessed January 10, 2021
Leave a Reply
You must be logged in to post a comment.

